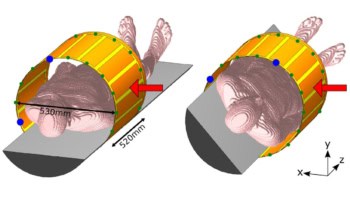
Body size has an influence on the dose conversion factors of a conventional chest posteroanterior (PA) examination for the organs in the field-of-view, except for the thyroid, according to an award-winning Belgian study presented last week at ECR 2018.
Body size has an influence on the dose conversion factors of a conventional chest posteroanterior (PA) examination for the organs in the field-of-view, except for the thyroid, according to an award-winning Belgian study presented last week at ECR 2018.
Previous studies have found similar results on the influence of the body mass index (BMI) or weight, and there is a growing consensus that using the automatic exposure control during a radiological examination will increase the exposure of overweight patients to maintain sufficient image quality.
“However, our study showed that the organ dose conversion factors decrease with increasing patient size,” noted lead author An Dedulle, a doctoral student in the department of imaging and pathology at the University of Leuven and also from the medical imaging software developer Qaelum, a spin-off company of the university. “This will result in a decreasing general conversion factor with increasing patient size: The radiation detriment of obese patients is lower than initially expected if only one, size independent, conversion factor would be used.”
This finding stimulates interest for patient-specific (organ) dose calculations in general radiography and should be considered in patient-specific reports of medical radiological procedures, the researchers explained in an e-poster that has received a prestigious magna cum laude award at ECR 2018.
The obesity epidemic
Nowadays, the radiation burden of the population is mostly an estimation based on general conversion factors (e.g., from dose area product to effective dose) for a reference normal-sized patient, but the prevalence of obesity has nearly tripled since 1975, and in 2008 more than 50% of the European population was overweight, according to Dedulle and colleagues.
The aim of their study was to examine the effect of BMI and water equivalent diameter (WED) on organ dose conversion factors in the case of conventional chest PA radiology examinations. They calculated dose conversion factors from voxel models made from total-body CT scans. All organs of importance could theoretically be included in the study, even though the current focus was chest PA imaging.
The study included 40 patients (20 female, 20 male) of different BMIs who underwent a CT exam from head to thighs. The researchers calculated the water equivalent diameter of every patient as the average WED over the central 20 cm of the axial CT slices in the lung region (from top to bottom of lungs).
They segmented the patients’ major radiosensitive organs: bones (for bone marrow and bone surface dose), thyroid, lungs, breasts, heart, liver, stomach, colon, kidneys, bladder, gonads, uterus (females)/prostate (males), skin, muscle, air inside the body, and the remainder. The team adjusted and configured an in-house developed Monte Carlo framework built for cone-beam CT for 2D radiography.
The researchers determined commonly used chest PA examination parameters from the dose monitoring system (Dose, Qaelum) in routine use at Leuven University Hospital, and they generated organ dose conversion factors for the typical, clinically used X-ray spectra and standard radiographic parameters.
The group used a statistical program (GraphPad Prism, GraphPad Software) to analyse and subsequently visualize the data and also analysed the female and male patients separately. The researchers tested normality and evaluated the influence of the BMI and water equivalent diameter on the organ dose conversion factors inside the field-of-view (red bone marrow, thyroid, lungs, heart and breasts) with two-tailed p-values with a confidence interval of 95% (p < 0.05).
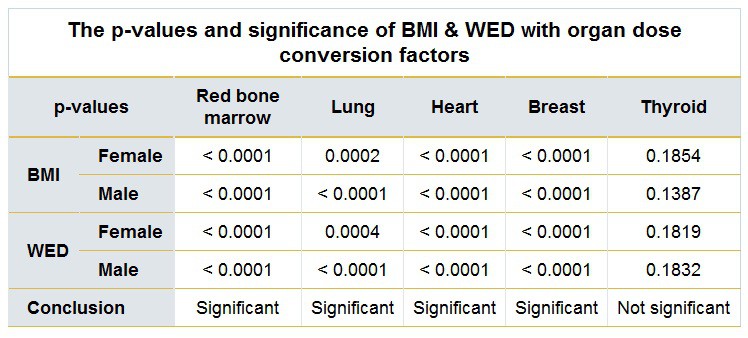
They observed significant linear correlations between the dose conversion factors and BMI, respectively WED, for both genders for the red bone marrow, lung, heart, and breast. The conversion factors fell with increasing BMI and WED, which can be explained by the extra shielding of the adipose tissue in patients with high BMI and WED. The researchers found nonsignificant results when correlating the BMI or WED with the thyroid dose conversion factors for both males and females (p > 0.05).
The results are summarized in the table below.
Study disclosures
The doctoral research of An Dedulle is supported by the Flanders Innovation & Entrepreneurship agency (grant number HBC.2016.0233). The work was conducted in cooperation with Qaelum and the University of Leuven.
- This article was originally published on AuntMinnieEurope.com.
© 2018 by AuntMinnieEurope.com. Any copying, republication or redistribution of AuntMinnieEurope.com content is expressly prohibited without the prior written consent of AuntMinnieEurope.com.